Microcomedones are the earliest, invisible stage of acne formation, developing deep within the hair follicle before any visible blackheads, whiteheads, or inflamed lesions appear. Their formation begins with subtle disruptions in the normal cycle of skin cell turnover. Under healthy conditions, keratinocytes lining the follicle shed in a controlled manner and exit the pore without obstruction. In acne-prone skin, this process becomes irregular, leading to the retention of dead skin cells داخل the follicle. At the same time, sebaceous glands may produce increased amounts of sebum, creating an environment where these cells can stick together and accumulate.



As this mixture of sebum and keratinized cells builds up, it forms a microscopic plug known as a microcomedone. At this stage, the blockage is not yet visible on the surface of the skin, but it alters the internal environment of the pore. The follicle may begin to expand slightly as material accumulates, setting the foundation for future acne lesions. Microcomedones are considered the starting point for all types of acne, meaning that both non-inflammatory comedones and inflammatory pimples often originate from this early structure.
Several biological factors contribute to microcomedone development. Hormonal influences, particularly androgens, can stimulate sebaceous glands to increase oil production, making it easier for dead skin cells to adhere داخل the follicle. Genetics may determine how efficiently skin cells shed and how prone the follicles are to blockage. In addition, changes in the composition of sebum can make it thicker or more likely to trap debris, further contributing to the formation of these microscopic plugs.
External and lifestyle factors can also influence this early stage. Environmental pollutants, sweat, and residue from skincare or cosmetic products may accumulate on the skin and mix with sebum, adding to the material داخل the pore. Inadequate cleansing or the use of occlusive formulations can increase the likelihood of buildup, while excessive or harsh exfoliation may disrupt the skin barrier and trigger compensatory oil production. Even habits such as frequently touching the face can introduce additional debris and microorganisms that contribute to pore congestion.
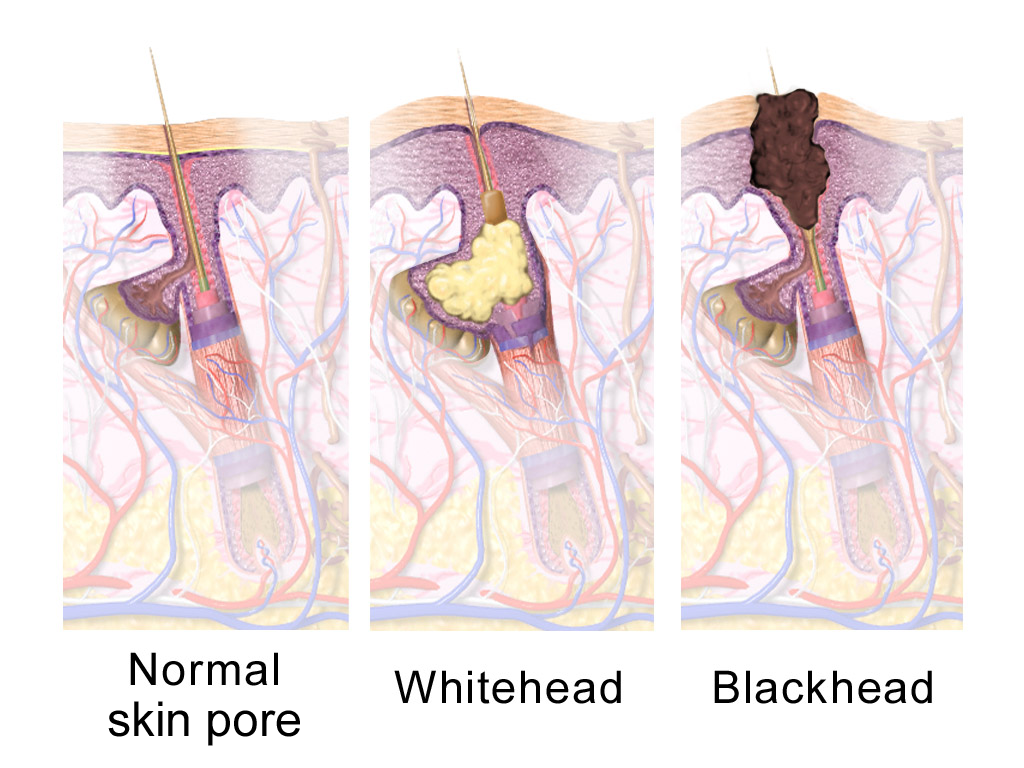
If microcomedones persist, they may evolve into visible lesions. When the follicular opening remains open, the contents can oxidize and form blackheads. When the opening is closed, the buildup forms whiteheads. Over time, the environment داخل the clogged pore may support the growth of acne-associated bacteria, potentially triggering inflammation and leading to papules or pustules. However, not all microcomedones progress, and some may resolve without becoming visible.
Managing microcomedone formation focuses on preventing the initial buildup داخل the follicle while maintaining skin barrier health. Topical retinoids are commonly used because they help normalize cell turnover and reduce the likelihood of dead skin cell accumulation. Salicylic acid may help exfoliate داخل the pore and dissolve excess oil, while niacinamide can support the skin by reducing inflammation and helping regulate sebum production. Gentle cleansing and consistent use of non-comedogenic products are also important in minimizing external contributors to pore blockage.
Because microcomedones are not visible, treatment often requires patience and consistency. Improvements may take time as the skin gradually clears existing blockages and prevents new ones from forming. Acne is influenced by multiple factors, including hormones, genetics, and environment, so results can vary. For persistent or worsening acne, consulting a qualified dermatologist may help guide a more targeted and effective approach based on individual skin needs.