In today’s fast-paced world, the desire for knowledge often competes with the demands of our daily lives.
We juggle work, family responsibilities, and social commitments, leaving little time for traditional education or self-improvement.
However, the rise of online courses has opened new doors, providing a pathway to learning that embraces flexibility and personal choice.
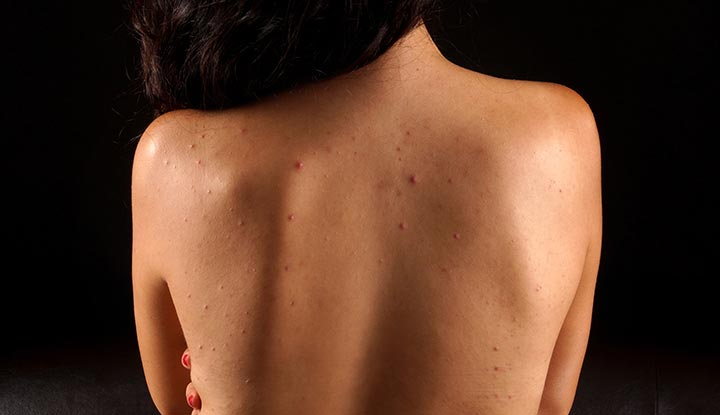
Acne on the back and chest, often referred to as truncal acne, develops through the same core biological mechanisms as facial acne. Increased sebum production, abnormal follicular keratinization, and the accumulation of dead skin cells within hair follicles contribute to clogged pores and the formation of microcomedones. As these blocked follicles enlarge, they may appear as blackheads or whiteheads. When inflammation develops in response to bacterial overgrowth and immune activation, papules, pustules, or deeper nodules can form. The skin on the back contains a high density of sebaceous glands, which partly explains why this area is especially prone to persistent breakouts.


Several contributing factors make back and chest acne more challenging to manage. Sweat, friction, and occlusion from tight clothing or athletic gear can trap heat and oil against the skin, promoting clogged pores. This mechanical irritation, sometimes described as acne mechanica, may worsen inflammatory lesions. Hormonal influences, particularly androgens, stimulate sebaceous glands and increase oil production, which can intensify both facial and truncal acne. Genetics also play a role, as some individuals naturally produce more sebum or have a stronger inflammatory response within the follicle.
Skincare habits significantly affect outcomes. Harsh scrubbing with abrasive tools may damage the skin barrier and increase inflammation without effectively clearing pores. Similarly, heavily fragranced body products or occlusive lotions may contribute to congestion in acne-prone individuals. On the other hand, insufficient cleansing after sweating may allow oil, bacteria, and dead skin cells to accumulate, increasing the likelihood of breakouts.
Evidence-informed treatment typically mirrors facial acne management but must account for the thicker skin and larger surface area of the trunk. Benzoyl peroxide is commonly used in body washes or leave-on treatments because it reduces Cutibacterium acnes and has anti-inflammatory effects. Wash-off formulations can be practical for covering broad areas, although they may bleach fabrics if not rinsed thoroughly. Salicylic acid may help exfoliate within pores and reduce blackheads and whiteheads by dissolving excess keratin and oil. Consistent use over several weeks is usually required before visible improvement occurs.
Topical retinoids can also be beneficial, as they normalize follicular keratinization and reduce microcomedone formation. However, applying prescription retinoids to large areas of the back may increase the risk of dryness and irritation, so gradual introduction and proper moisturization are important. Lightweight, non-comedogenic moisturizers containing ingredients such as ceramides or niacinamide may support barrier function without contributing to clogged pores.
For individuals with widespread, painful, or scarring lesions, professional evaluation is advisable. Dermatologists may consider oral antibiotics for moderate inflammatory acne, hormonal therapies when indicated, or oral isotretinoin for severe, treatment-resistant cases. Early intervention is important because truncal acne has a higher tendency to leave post-inflammatory hyperpigmentation or permanent scarring due to deeper inflammation and delayed treatment.
Lifestyle adjustments may also reduce flare-ups. Showering soon after sweating, wearing breathable fabrics, and minimizing friction from tight straps or backpacks can help decrease mechanical irritation. Avoiding aggressive physical exfoliation and instead using gentle chemical exfoliants may provide more controlled improvement in clogged pores.
Improvement in back and chest acne generally occurs gradually. Visible reduction in lesions may take several weeks, and consistent maintenance is often necessary to prevent recurrence. Because skin on the trunk can be both thicker and more reactive, balancing active treatments with barrier support is essential. When acne persists, worsens, or begins to scar, consultation with a qualified healthcare professional can help tailor therapy and minimize long-term skin changes.