Post-inflammatory hyperpigmentation (PIH) develops as a biological response to skin inflammation, particularly in conditions such as acne where the skin barrier and deeper layers are disrupted. When an acne lesion forms, inflammatory signals trigger melanocytes, the pigment-producing cells in the basal layer of the epidermis, to increase melanin production. This process is part of the skin’s protective response, as melanin can help shield tissue from further damage. However, the excess pigment is not always distributed evenly, leading to localized darkened areas that remain after the visible acne lesion has healed.

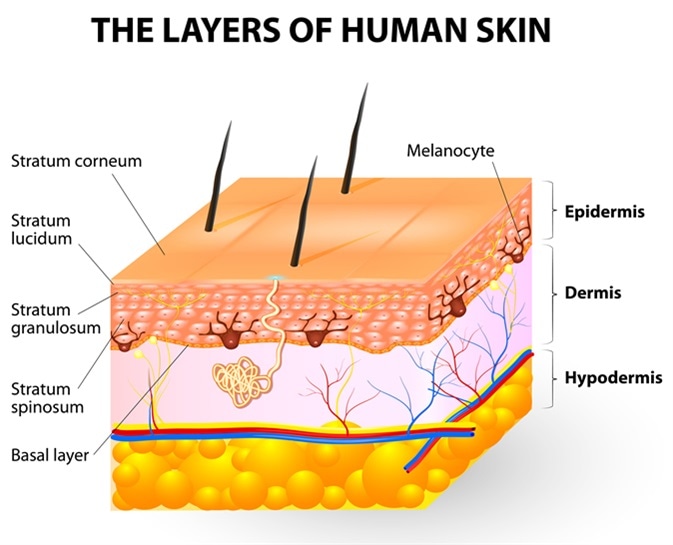

The depth of inflammation plays a key role in determining how PIH appears and how long it lasts. When inflammation is limited to the epidermis, excess melanin accumulates in the upper layers of the skin, typically resulting in light brown to dark brown marks that may gradually fade over time. If inflammation extends deeper into the dermis, pigment can be deposited in the dermal layer, often appearing as bluish-gray discoloration and taking significantly longer to resolve. This explains why more severe or persistent acne lesions are more likely to leave noticeable marks.
Several contributing factors influence the likelihood and severity of PIH. Skin types with higher baseline melanin levels are generally more prone to developing hyperpigmentation because melanocytes are more reactive to inflammatory signals. Repeated irritation, whether from aggressive skincare routines, overuse of active ingredients, or physical manipulation مثل picking or squeezing, can prolong inflammation and stimulate continued melanin production. Environmental exposure, particularly ultraviolet radiation, can further darken existing marks by activating melanocytes and increasing pigment synthesis.
Managing PIH involves both preventing excess pigment formation and supporting gradual skin renewal. Controlling acne-related inflammation is essential, as fewer active lesions reduce the triggers for pigmentation. Ingredients such as niacinamide may help regulate pigment transfer and calm inflammation, while azelaic acid is often used for its ability to address both acne and uneven pigmentation. Gentle exfoliating agents, including certain alpha hydroxy acids, can support the removal of pigmented surface cells over time. Retinoids are also commonly incorporated to promote cell turnover and improve overall skin texture.
Sun protection plays a critical role in preventing PIH from worsening. Broad-spectrum sunscreen can help limit UV-induced melanocyte stimulation, allowing existing marks to fade more predictably. Without consistent sun protection, even effective treatment strategies may yield slower or less noticeable improvement.
Post-inflammatory hyperpigmentation is not a true scar but rather a pigmentary change resulting from inflammation. While it can persist for weeks or months, especially in deeper or more severe cases, it often improves gradually with consistent care. A balanced approach that minimizes irritation, protects the skin from additional damage, and supports controlled cell turnover is typically the most effective way to manage and reduce its appearance over time